It’s important to do a comparison of Lyme disease vs. multiple sclerosis (MS) as the two do have much in common. At the same time, they both have their own unique differences that distinguish one from another.
Lyme disease is caused by a bite from a deer tick or black-legged tick, which transfer Borrelia burgdorferi bacteria. The longer a tick is attached to you, the higher your risk of developing Lyme disease is.
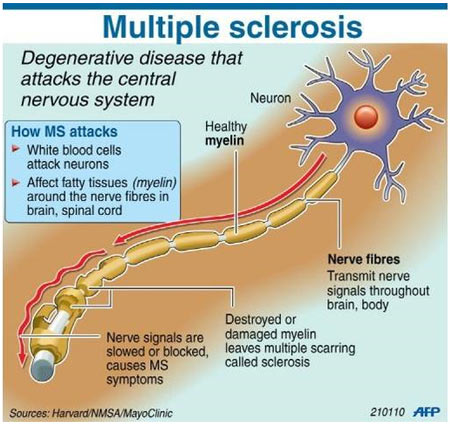
Multiple sclerosis is an autoimmune disorder in which the body’s immune system attacks the myelin, a protective coating around the nerves and spinal cord. As myelin deteriorates, it damages the nerves and spinal cord, thus causing the MS symptoms.
Lyme disease may present itself like multiple sclerosis, but there are distinctive differences, which we will outline to help you decipher between the two.
Lyme disease and MS: Often confused
In order to get a definite diagnosis of either Lyme disease or multiple sclerosis, doctors will have to conduct several tests, including blood tests, to confirm diagnosis of either one. Symptoms alone may be quite confusing.
Although it is unlikely that a patient has both Lyme disease and MS, the possibility is still there. Lyme disease symptoms may appear like multiple sclerosis, causing confusion at first. It is only with an MRI scan and spinal tap that the doctors can confirm or deny a diagnosis of multiple sclerosis.
Lyme disease vs. MS: U.S. prevalence
Multiple sclerosis: Majority of MS patients are diagnosed between the ages of 20 to 40, but it can develop at any age. There are over 400,000 cases of multiple sclerosis in the U.S., with women accounting for the majority of cases. Each week, there are an additional 200 cases of multiple sclerosis diagnosed in America.
There are roughly 30,000 Lyme disease cases reported annually, but it’s not an accurate reflection of how many cases actually occur, as these are incidences only reported to the Centers for Disease Control and Prevention.
In order to improve data collection on Lyme disease, the CDC has set out two different studies known as Project 1 and Project 2. Project 1 estimated 228,000 cases of Lyme disease through laboratory testing, and Project 2 estimated 329,000 cases of Lyme disease based on claims from medical insurance databases.
Lyme disease vs. MS: Signs and symptoms
Symptoms of multiple sclerosis include:
- Numbness or weakness in one or more limbs
- Partial or complete vision loss, pain during eye movement
- Prolonged double vision
- Electric-shock sensations with certain neck movements
- Tremor, lack of coordination
- Slurred speech
- Fatigue
- Dizziness
- Problems with bowel and bladder functions
Early signs of Lyme disease include:
- Fever
- Chills
- Headache
- Muscle and joint pain
- Swollen lymph nodes
- Erythema migrans rash, which looks like bull’s eye
As the disease progresses, symptoms can worsen into severe headache and neck stiffness, with additional rashes, arthritis accompanied by severe joint pain and swelling, muscle loss in the face, intermittent pain in the tendons, muscle joints, and bones, heart palpitations or irregular heartbeat, dizziness or shortness of breath, nerve pain, shooting pain, numbness or tingling, and problems with short-term memory.
Lyme disease vs. MS: Causes and transmission
Lyme disease is caused by a bite from the Ixodes scapularis, or deer tick. These ticks are not inherently infected with Lyme disease, but rather they get it from feeding on an affected animal. These ticks can be found in wooded lands and prefer damp areas underneath trees. Because ticks are so tiny, it is difficult to notice that they are on you, let alone that they bite you, so it’s important that you cover your body and check yourself every so often if you are going out for a hike.
Tick populations are higher in the East, Midwest, and West coast, but can be found all across the U.S.
There is some debate about how long it takes a tick to infect a person. Some experts suggest it’s up to 24 hours from attachment, and others believe it’s even less than that. Essentially, the longer a tick is attached to you, the higher your risk of developing Lyme disease is.
The cause for multiple sclerosis is largely unknown, but what is known is that it is an autoimmune disease in which the body’s own immune system begins to wrongfully attack itself. In multiple sclerosis, the target for attack is the myelin, which is the protective coating around nerve fibers and the spinal cord. Genetic and environmental factors have been credited as possible causes for multiple sclerosis.
Lyme disease vs. MS: Risk factors
One of the risk factors for Lyme disease is being in wooded, grassy areas for prolonged periods of time, especially in the Northeast and Midwest parts of America where deer ticks are more prevalent. Other risk factors include exposing skin in such environments and not removing a tick properly once one has latched onto you. As mentioned, the longer the tick is attached, the greater the risk of Lyme disease.
Risk factors for multiple sclerosis include age, being female, having a family history of multiple sclerosis, having certain infections like Epstein-Barr, being white or of Northern European descent, living in temperate climates, already having another autoimmune disease, and smoking.
Lyme disease vs. MS: Complications
Complications can arise in both Lyme disease and multiple sclerosis if not managed and treated properly. If Lyme disease is caught early, antibiotics can be given immediately to reduce complications, but if treatment is delayed chronic complications can arise including fatigue, arthritis and joint pain, headaches, short-term memory problems, numbness, Bell’s palsy (facial paralysis), heart problems including slow or irregular heartbeat, and depression, which can be set off by living with the complications of Lyme disease.
Complications of multiple sclerosis include an increase in urinary tract infections due to disrupt bladder nerves responsible for opening and closing of the bladder, osteoporosis, pressure sores, aspiration pneumonia which can make swallowing difficult and so food and liquid spills into the lungs, and depression as a result of living with multiple sclerosis. Many multiple sclerosis treatments can help prevent these complications from arising so it’s important to get proper treatment right away.
Lyme disease vs. MS: Diagnosis and treatments
Diagnosing Lyme disease involves looking for the erythema migrans rash, which is reported in 70 percent of Lyme disease cases. Your doctor will also evaluate your symptoms and confirm the diagnosis with blood work.
For Lyme disease treatment, your doctor will put you on a regime of antibiotics, which may be taken for several weeks. It’s important that you completely finish your antibiotics, even if you start feeling better. Take note that some antibiotics may make your skin more sensitive to the sun, so you should avoid being out in the sunlight for prolonged periods of time.
Diagnosing multiple sclerosis involves evaluating a patient’s family history and symptoms. If multiple sclerosis is suspected, your doctor has many testing options including an MRI scan, a spinal tap, blood tests, and evoked potential tests, which record electrical signals produced in response to a stimuli.
Treatment for multiple sclerosis can utilize corticosteroids, plasma exchange (in which the plasma is removed from blood cells, mixed with a protein solution, and put back into the body), medications to help manage symptoms and prevent relapse, physical therapy, muscle relaxants, medications to reduce fatigue, and other medications for depression, sexual dysfunction, bladder troubles, and other symptoms associated with multiple sclerosis.
Working closely with your doctor can help determine the best treatment methods for your needs and symptoms in order to live a life as normal as possible with multiple sclerosis.
Source: http://www.belmarrahealth.com/lyme-disease-vs-multiple-sclerosis-ms-differences-in-symptoms-causes-and-treatment/
*Disclaimer: The views and opinions expressed in this article are those of the authors and do not necessarily reflect the official policy or position of LymeNow or the LymeNow community.